H. Freya, A. Lahtinenb, T. Heinonenb, and P. Dastidarc
1. Remarks on Advances of Radiological Techniques in Neurology
Radiological techniques started to contribute relatively late in clinical neurology after the original discovery
of x rays in 1895 by Roentgen. The application of conventional skull x-ray techniques improved the diagnosis
and treatment of skull traumas. But first the development of pneumo-encephalography for the study of the soft tissues
and ventricles in the brain and myelography after injection of air or inert gas into the CSF space started a new
stage of development. These techniques were slowly substituted after late fiftees by the introduction of contrast
media (aortocervical and later selective angiographies and water insoluble and later water soluble opaque contrastmedia
for myelography.
A new and revolutionary stage of the imaging techniques in neuroradiology and neurology started, when Hounsfield
and Cormack developed CT (computerized tomography) and received a Nobel price in 1972. CT uses ionizing radiation,
but it has no other major risks and is relatively comfortable for the patient. Until the development of spiral-
techniques and 3D modelling the CT slices have been limited primarily to transaxial views. In CT images are generated
by passing an xray beam through the skull or other object (e.g. spine and vertebral column) and measuring its
degree of attenuation. The ability to attenuate x rays of different tissues (e.g. brain, bone and CSF differs
and can be measured numerically as a tissue density number for each voxel (volume element). These numbers can be
converted to gray scale values and presented visually as pixels. A large number of reconstruction and filtering
techniques are nowadays available to improve the quality of the pictures and thus also the diagnostics. The use
of CT contrast media further improves the differential diagnostics.
MRI (Nuclear magnetic resonance imaging) is rapidly substituting CT as the best structural neuroimaging technique.
MRI has also potential for the study of the biochemistry and physiology of the nervous system. In fact the principles
of MRI are older than those of CT. The MR phenomenon was demonstrated already in 1946 by Bloch and Purcell. They
got a Nobel price for this discovery in 1952.
However the first clinical applications in radiology appeared in the seventies. In MRI the object (head etc)
is placed in a high field strength magnetic field ( from 0.5 to 1.5 Tesla usually). This concentrates the magnetic
moment of individual protons and the net magnetic moment is then tipped by sending radio-frequency signals that
excite the tissue. After this the protons relax again and return to their original position. Different relaxation
times (T1 and T2) as well as proton density are measured and can be further manipulated by using various pulse
sequences. Several quantum leaps have been made during eightees and ninetees in MRI techniques (e.g. Fast spin
echo (FSE), high performance gradients, echo planar and diffusion weighted imaging , MR contrast agents and CSF
fluid velocity analysis and introduction of interventional MRI).Bradley WG and Bydder GM, 1997.
The possibility to vary the components of the MR signal and the type of image generated improve the clinical
applicability of MRI considerably especially for identifying pathological tissue. Thus the tissue resolution of
MRI is far superior to the CT except for bone.
The introduction of MR contrast media has further widened the clinical applicability of MRI into MR angiography.
MRI is also widening its applicability through such techniques as magnetic spectroscopy and echo planar imaging
to measure tissue metabolism, physiology and cerebral blood flow.
2. Clinical Application of MRI Image processing in Neurology
It is imposssible to describe all the clinical applications of the abovementioned techniques in this context.
One can only refer to a number of textbooks; e.g. Osborn NA 1994, Gonzalez et al. 1985, Taveras, J.M. Neuroradiology
(third ed.) 1996, Bradley WG Jr and Bydder, GM 1997.
In general the first clinical applications were mainly finding of space occupying lesions (expanses and tumors
in brain, as well as brain infarcts, intracerebral and other intracranial haemorrhages ).
MRI is much more sensitive than CT to be used in the analysis analysis of tissue pathology; in evaluation of
degenerative and atrophic processes (ventricular and sulcar enlargement and cortical atrophy ). White matter plaques
in multiple sclerosis, diffuse ischemia and infarction, haemorrhages, differential diagnosis of tumors, developmental
anomalies and congenital malformations.
In addition to the structural changes in brain due to normal aging especially in dementias MRI has become an
important auxiliary diagnostic tool.
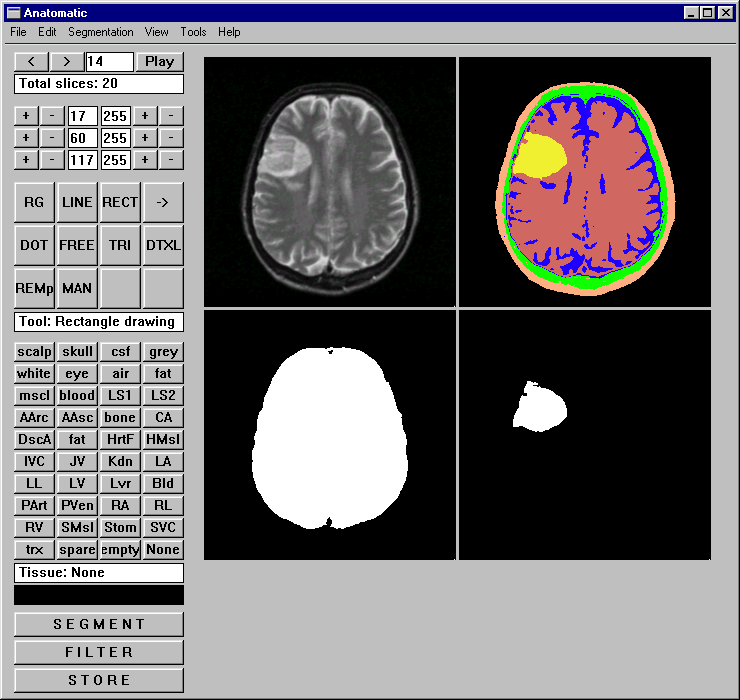
Figure 1. In vascular dementias ischemic changes aswell as leucoaraiosis in periventricular
white matter in addition to multiple infarcts help to right diagnosis.
In dementia of Alzheimer type the neurodegenerative changes particularly in hippocampus (volumetry) and related
areas in temporal and parietal cortex , where also neuropathological postmortem changes are usually most profound
help to make the right diagnosis. More recently such dementia entities as frontal lobe dementia and Lewy body dementia
have been added among the differential diagnostics based partially on MRI. In Huntington´s disease patterns
of hypometabolic activity are found in the basal ganglia of both the patients and their relatives in risk. FMRI
can in near future be used in the diagnosis of Parkinson's disease and other extrapyramidal disorders. Recent
findings of structural changes seen in MRI in schizophrenia are giving new light to the possible underlying pathology
and probable early developmental lesions in this disease.
3. Recent Advances in the Development and Application of
3.1 Neuroimaging Methods in Neurology
The increasing use of different computer based imaging methods, multimodal imaging and 3D modelling and fusion
of different imaging methods with each others have made new developments and application for use also in clinical
applications possible. For these new developments are responsible especially the research initiatives, which have
emerged after the publication of the Mapping the Brain and its functions report in U.S.A. (Poscura P and Martin
J, 1992). For overviews in the recent developments see e.g. Toga AW and Mazziotta JG 1996 , Frackowiak RSJ et al.
1997.
3.2. Digital neuroatlases and their application
There exist several different ways and tools for building human ( or animal ) brain atlases.
Atlas is a special form of map that incorporates stereotactic elements. Computerized stereotactic atlases are becoming
more important for the localization and segmentation of human brain anatomy and physiology. Some of the tools available
to analyse brain structures and functions at macroscopic level are listed in Table I.
Table I. Tools for macroscopic study of the brain
CT
MRI
MR spectroscopy (combined with topography)
SPECT
PET
EEG
MEG
Evoked potentials
Postmortem cryosectioning combined with staining
Multimodal imaging
____________________________
The most straightward approach is based on the use of only one fixed parameter for spatial normalization. E.g.
shape and adjust the size (MRI image or section). Here in comparisons between different approaches the so-called
densitometric approach seems to be the most reliable method sofar. Instead of this Talairach and Tournoux used
anterior and posterior brain commisures as reference points.
Segmentation is a third alternative e.g. to separate white matter from gray matter or ventricles (CSF space).
Brain image segmentation is especially well suited for this type of an approach.
Visualization is helpful especially in multimodal imaging atlases (fusions), where different colours can be
painted over a grey scale.
The probabilistic approach means, that a large population of samples is treated statistically and medians of
these digital samples are represented as standards. E.g. at the Montreal Neurological Institue a MRI brain atlas
was created by combining MRI images taken from 305 normal 28 year old individuals. After this a median stereotactic
digital neuroatlas was developed. (Evans AC et al. 1992).
One has to keep in mind, that a brain atlas is essentially also a database. By combining the other existing
information with different types of databases (books, articles etc.) it is possible to increase enormously the
efficiency of a digital neuroatlas.
We in Tampere have developed a different type of an approach. The original digital neurotlas is transferred
on the corresponding sections of the MRI image of the patient The shape and size of the neuroatlas can be modified
by using different mathematical algorithms (rubber sheet and wrap algorithms). Also the possible errors in the
patient image (rotations, translations and stretching) can be corrected (Lahtinen A et al 1998). Some of the neuroatlases,
which can be found in Internet are listed in Table II.
Table II. Neuroatlases in Internet
Talairach Tournoux Brain Atlas
Talairach Tournoux Referential Brain Atlas
Brodman Gyri Brain Atlas
SchaltenBrand Wahren Brain Atlas (axial-, coronal-, sagittal slices.
Ono Kubik Sulcal Atlas (indexed)
The whole brain atlas
Atlas at Washington
Ito´s Brain Atlas
PET Brain Atlas
Atlas of Brain perfusion SPECT
The Human Brain: Dissections of the Real Brain
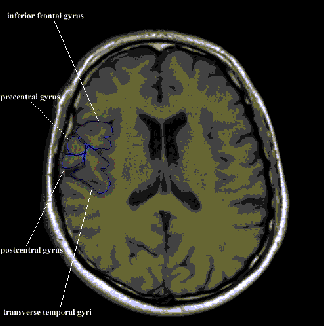
Figure 2. An example of the Tampere Brain Atlas to illustrate a brain infarct in the
right a.cerebri media lesioning inferior frontal gyrus, both precentral and postcentral gyri and inferior parietal
gyrus.
A second example of the use of neuroatlas, which shows an brain haemorrhage in a 3D axial serial section image
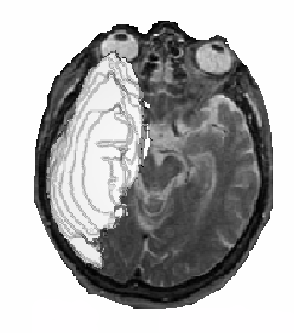
Figure 3. 3D image of a large haemorrage. This type of image can be used e.g. in planning
of neurosurgery.
A third example is the localization of multiple sclerosis plaques in the white matter of brain after segmentation
(Fig 4). This type of an approach is currently used to follow the possible effect of beta-interferon treatment
of MS patients (Dastidar P. et al. 1999).
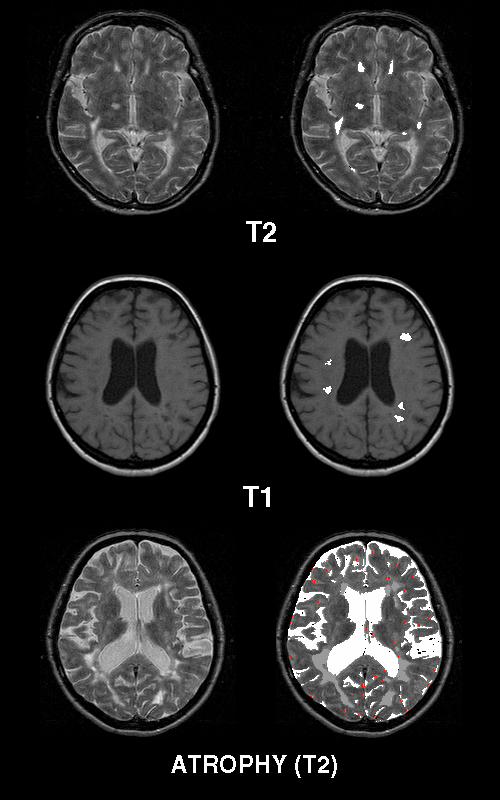
Figure 4. Axial T1 and T2 weighted MRI sections of MS plaques and brain
atrophy.
However there are still problems transforming brains to a common atlas. Because of the individual variance and
changes due to ageing the accuracy of brain atlases is restricted to limited regions of the
Brain. Especially cortex is problematic in this sense (Benayoun et al. 1994). Subcortical areas are more homologous
and the points here are more easily identifiable (Kazanovskaya et al. 1991).
3.3 Application of fMRI in Clinical Neurology
fMRI trechniques are noninvasive, multiple, longitudinal. When compared with other functional
brain imaging techniques (EEG, PET, magnetic source imaging and near infrared spectroscopic imaging, fMRI has good
temporal resolution and excellent spatial resolution. Therefore it has become a new and very powerful research
tool (Karni, A. et al. 1995) and has started to show considerable clinical benefit while studying the underlying
pathology in different brain diseases. In future it may also be used to follow up the recovery of the brain lesions
and be used to help in restorative neurology for higher cognitive functions.
In most fMRI studies, image sets are acquired while the patient is alternatively in an active
and control state. While changes in cerebral blood flow and its oxygenation degree are measured. In the near future
these types of techniques can also be applied to study the possible regional pathological changes related to CBF.
In this connectiion fMRI has to be compared with diffusion imaging EPI techniques and SPECT or PET.
3.4. Clinical Applications of Volumetric image Analysis in Neurology
Despite of the still existing difficulties in practical application of volumetry these techniques
have already been set widely to study such degenerative diseases of the brain as Alzheimer-type dementia (Erkinjuntti
et al. 1993, Devernoy 1998). Brain tumors (Velthuizen et al.1995), brain infarcts (Heinonen et al.1998) and intracerebral
hematomas (Dastidar et al.1997) aswellas MS plaques (Dastidar et al.1999).
In the near future 3D visualization will become a valuable tool for this type of applications
in clinical neurology and planning of stereotactic neurosurgery, radiotherapy and follow up of the effect of treatment.
(Heinonen et al.1998).
4. Some Future Prospects and needs
Especially in clinical neurosurgery the use of stereotactic methods, when combined with 3D modelling
would benefit the planning and surgical treatment immensely. The same is due to radiotherapy of brain tumors. The
future applications of fMRI and multimodal imaging techniques will open up totally new ways to understand the cognitive
and psychiatric disorders. The combination of these techniques with already existing international databases and
their use will also improve the diagnostics and treatment of brain and other nervous system disorders much. At
the same time the need to educate new clinical neuroscientists and clinicians who can understand and use these
techniques will become an absolute necessity. In fact it is necessary to train a new generation of specialists
to fulfil all these demands.
References
[1] Osborn A.G.: Diagnostic neuroradiology. Mosby Press.Mosby Year Book Inc.1994.
[2] Gonzalez et al., Head & spine imaging. Wiley Medical Press.1985.
[3] Taveras, J.M., Neuroradiology, Third ed. Williams and Wilkins Press.1996. .
[4] Bradley W.G.Jr. and Bydder G.M., Advanced MR Imaging techniques. Martin Dunitz LTD, London. 1997.
[5] Talairach J. and Tournoux P. Co planar stereotaxic atlas of the human brain. 1988. Thieme, New York.
[6] Evans AC, Collins Dl and Milner B., An MRI based stereotactic brain atlas from 300 young normal subjects.
Proc. 22nd Ann.symposium of the society of neuroscientists, Anaheim, 1992.
[7] Poscura J. and Martin J.Mapping the human brain and its functions. Institute of Medicine. 1992.
[8] Toga AW and Mazziotta JC. Brain mapping, the methods. Academic Press.1996.
[9] Frackowiak RSJ, Friston, KJ.,Frith CD, Dolan RJ and Mazziotta JC.: Human brain function. Academic Press 1997.
[10] Lahtinen A.,Kulkas,T.,Heinonen T. and Frey H.: The application of a new digital neuroatlas for post-stroke
dementias. Norage 1998 Proc. 86,1998.
[11] Dastidar P., Heinonen T. Vahvelainen T.Elovaara I and Eskola H.: Computerized volumetric analysis of lesions
in multiple sclerosis using a new semiautomatic segmentation software. Med. Biol. Engineering & computing.
37: 104 107. 1999.
[12] Benayoun S., Ayache N. and Cohen I.: An adaptive model for 2D and 3D dense non-rigid motion computation. INRIA
Inter.Rep. No 2297, 1994.
[13] Kazarnovskaya MI., Borodkin SM., Shablov VA., Krivosheina VY and Golanov AV.: 3 D computer model of subcortical
structures of human brain. Comput.Biol.Med. 21(6),451-457, 1991.
[14] Karni A., Meyer P., Jezzard M, Adams M, Turner R. and Ungerleider LG.: Functional MRI evidence for adult motor
cortex plasticity during motor skill learning. Nature 377,155-158 (1995)
[15] Erkinjuntti T.,Lee D.,Gao F.,Steenhuis R.,Eliasziw M.,Fry R.,Merskey H and Hachinski V.: Temporal lobe atrophy
on magnetic resonance imaging in the diagnosis of early Alzheimer´s disease. Arch.Neurol.50, 305-310.1993.
[16] Duvernoy H.: The human hippocampus.2.ed. Springer Verlag Berlin Heidelberg.1998.
[17] Velthuizen R.,Clarke L.,Phuphanics S.,Hall O.,Bensaid A.,Arrington J.,Greenberg HM. And Silbiger M.: Unsupervised
measurement of brain tumor volume on MR images.J.Magnetic Resonance Imaging.5.594-605.1995.
[18] Heinonen T, Dastidar P.Eskola H., Frey H., Ryymin P and Laasonen E.: Appplicability of semi-automatic segmentation
for volumetric analysis of brain lesions.J.Med.Eng.Technol.22.173-178.1998.
[19] Dastidar P, Heinonen T., Virta T., Ryymin P. and Kuurne T.: Evaluation of operative treatment of intracerebral
hematomas by semiautomatic segmentation method. Proc. 9th int.conference.Biomed.Engineering.Singapore.733.1997.
[20] Heinonen T., Visala K., Blomqvist M., Eskola H. and Frey H.: 3Dvisualization library for multimodal images.
Comp.Med.Imaging and Graphics.22.267-273.1998.

 Home
Current Issue
Table of Contents
Home
Current Issue
Table of Contents




